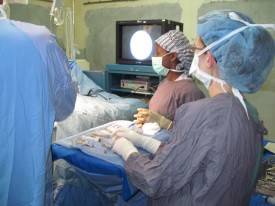
African Pediatric Neurosurgery: Statistics and Needs
Africa has approximately one billion people and 1200 neurosurgeons; 857 in North Africa, 160 in South Africa, and 142 in sub-Saharan Africa with a population of 723 million people (1 neurosurgeon per 5 million people), including an estimated 19 countries with zero neurosurgeons. Moreover, approximately half the population in most African countries is less than 18 years old, and there are only 12 to 15 pediatric neurosurgeons on the continent. That dearth is attributable primarily to the near absence of pediatric neurosurgeons on academic faculty, and to a lesser extent, to the fact that African neurosurgeons prefer to treat patients with more lucrative conditions.
In addition, hydrocephalus in Africa has reached epidemic proportions, primarily due to the high risk of perinatal infections and the high prevalence of congenital disorders such as spina bifida. A majority of hydrocephalic children do not receive treatment and die before their second birthday. Given the scarcity of neurosurgeons in the region and the economic and infrastructural constraints, timely treatment of these patients presents an enormous challenge.
Among the proposals to confront Africa’s hydrocephalus epidemic is additional training for current African neurosurgeons. Examples include large scale efforts from the Foundation for International Education of Neurosurgeons (FIENS), the International Society of Pediatric Neurosurgeons, and the Walter E. Dandy Neurosurgical Society, and personal efforts such as those of Benjamin Warf in Uganda, and Leland Albright and Susan Ferson in Kenya. Although African neurosurgeons lack training in pediatric neurosurgery, many of them currently care for children. Providing additional training in hydrocephalus is valuable, yet this strategy alone leaves gaps in other common congenital conditions including spina bifida and encephaloceles. Thus any long-term approach to supplying good neurosurgical care to sub-Saharan Africa must address the lack of educational opportunities for training pediatric neurosurgeons. This must be confronted by building self-sustaining pediatric neurosurgical departments.
Africa has approximately one billion people and 1200 neurosurgeons; 857 in North Africa, 160 in South Africa, and 142 in sub-Saharan Africa with a population of 723 million people (1 neurosurgeon per 5 million people), including an estimated 19 countries with zero neurosurgeons. Moreover, approximately half the population in most African countries is less than 18 years old, and there are only 12 to 15 pediatric neurosurgeons on the continent. That dearth is attributable primarily to the near absence of pediatric neurosurgeons on academic faculty, and to a lesser extent, to the fact that African neurosurgeons prefer to treat patients with more lucrative conditions.
In addition, hydrocephalus in Africa has reached epidemic proportions, primarily due to the high risk of perinatal infections and the high prevalence of congenital disorders such as spina bifida. A majority of hydrocephalic children do not receive treatment and die before their second birthday. Given the scarcity of neurosurgeons in the region and the economic and infrastructural constraints, timely treatment of these patients presents an enormous challenge.
Among the proposals to confront Africa’s hydrocephalus epidemic is additional training for current African neurosurgeons. Examples include large scale efforts from the Foundation for International Education of Neurosurgeons (FIENS), the International Society of Pediatric Neurosurgeons, and the Walter E. Dandy Neurosurgical Society, and personal efforts such as those of Benjamin Warf in Uganda, and Leland Albright and Susan Ferson in Kenya. Although African neurosurgeons lack training in pediatric neurosurgery, many of them currently care for children. Providing additional training in hydrocephalus is valuable, yet this strategy alone leaves gaps in other common congenital conditions including spina bifida and encephaloceles. Thus any long-term approach to supplying good neurosurgical care to sub-Saharan Africa must address the lack of educational opportunities for training pediatric neurosurgeons. This must be confronted by building self-sustaining pediatric neurosurgical departments.
|
The Kenya initiative, by Leland Albright and Susan Ferson
Leland Albright, MD and his wife Susan Ferson, RN, PNP, moved to Kijabe, Kenya, in September 1, 2010, to practice and teach pediatric neurosurgery. When the Albrights arrived in Africa, they believed it would take between 2-3 years to establish a self-sustaining pediatric neurosurgery department at the AIC Kijabe Hospital. However, after a few months, it became clear that it would probably require at least 6 years to reach that goal. Dr. Albright is starting his fourth year in Kenya, doing an excess of 100 major neurosurgical cases per month. Since arriving, Dr. Albright established a one-year fellowship in pediatric neurosurgery that has been supported by the Medtronic Foundation and the International Society of Pediatric Neurosurgery, and validated by the University of Nairobi. Ugandan neurosurgeon Humphrey Okechi, completed the fellowship in November 2011 and has become a consultant on the Kijabe hospital staff. In addition, neurosurgeon Teddy Totimeh will begin his fellowship in pediatric neurosurgery March 1, 2014 |
 Dr. Okechi with Leland Dr. Okechi with Leland
Who are Leland and Susan
Dr. Albright taught and practiced pediatric neurosurgery for 25 years at the Children's Hospital of Pittsburgh, Pennsylvania, and for four years at the University of Wisconsin Health Center in Madison, WI. He is the senior editor of the premier textbook of pediatric neurosurgery, and a world authority on neurosurgical treatments of movement disorders in children. Susan practiced as a nurse for 14 years and a pediatric neurosurgery nurse practitioner for an additional 12 years before moving to Kijabe. She is nationally recognized for her expertise in treating spasticity using baclofen pumps. Learn more about Leland and Susan at their blog. Who is Dr. Okechi Humphrey Okechi is a Ugandan physician who completed his neurosurgical training in China in 2010. He completed his fellowship in pediatric neurosurgery with Dr. Albright in 2011 and is his colleague in pediatric neurosurgery. He has played an instrumental role at AIC Kijabe Hospital by providing continuity of clinical care and neurosurgical training for residents and fellows. |
 Dan and Naomi Ochieng
Dan and Naomi Ochieng
Who are the Ochiengs
Dan and Naomi Ochieng are two outstanding Kenyan physicians who have been neurosurgery residents in the University of Nairobi program for the past three years and who have had meaningful rotations with Leland and Susan in Kijabe. Dan recently received an AANS/CNS Traveling Fellowship in Pediatric Neurosurgery and spent three months at the Boston Children's Hospital. Dan and Naomi felt their experience in Nairobi did not provide the caliber of neurosurgical training that would be needed for their career in Kijabe, and on January 1, 2014 both began the five-year neurosurgery residency at the University of Cape Town, under the direction of Dr. Graham Fieggen, perhaps the premier neurosurgery residency in Africa.
Goals of the Kenya Initiative
Leland and Susan have established a unique Pediatric Neurosurgery center that cares for thousands of children in Sub-saharan Africa. The goal of the Kenya Initiative is to provide continued high quality pediatric neurosurgical care and training after Leland and Susan leave, probably September 1, 2016. Dan and Naomi Oohing have committed to return to Kijabe after completion of their neurosurgical training in South Africa on December 31, 2018. In the interim, Leland's colleague Dr. Okechi will continue his neurosurgical practice in Kijabe. Between September 2016 and January 2019 he will require pediatric neurosurgical assistance to complete the 100+ operations that are needed each month. Another goal is to continue to provide education in pediatric neurosurgery to residents rotating in Kijabe from the University of Nairobi and to provide on-going year-long fellowships in pediatric neurosurgery.
Dan and Naomi Ochieng are two outstanding Kenyan physicians who have been neurosurgery residents in the University of Nairobi program for the past three years and who have had meaningful rotations with Leland and Susan in Kijabe. Dan recently received an AANS/CNS Traveling Fellowship in Pediatric Neurosurgery and spent three months at the Boston Children's Hospital. Dan and Naomi felt their experience in Nairobi did not provide the caliber of neurosurgical training that would be needed for their career in Kijabe, and on January 1, 2014 both began the five-year neurosurgery residency at the University of Cape Town, under the direction of Dr. Graham Fieggen, perhaps the premier neurosurgery residency in Africa.
Goals of the Kenya Initiative
Leland and Susan have established a unique Pediatric Neurosurgery center that cares for thousands of children in Sub-saharan Africa. The goal of the Kenya Initiative is to provide continued high quality pediatric neurosurgical care and training after Leland and Susan leave, probably September 1, 2016. Dan and Naomi Oohing have committed to return to Kijabe after completion of their neurosurgical training in South Africa on December 31, 2018. In the interim, Leland's colleague Dr. Okechi will continue his neurosurgical practice in Kijabe. Between September 2016 and January 2019 he will require pediatric neurosurgical assistance to complete the 100+ operations that are needed each month. Another goal is to continue to provide education in pediatric neurosurgery to residents rotating in Kijabe from the University of Nairobi and to provide on-going year-long fellowships in pediatric neurosurgery.
Ways you can help
With countless needs and limited resources, there are many ways to contribute to the Kenya Initiative. Consider volunteering for the neurosurgery service at AIC Kijabe Hospital. Pediatric neurosurgeons and senior-level neurosurgery residents are invited to help provide clinical care and teaching. Second, consider offering financial support for Dan and Naomi as they complete their training in Cape Town. Lastly, there is an incredible need for medical equipment throughout the hospital. AIC Kijabe Hospital is a non-profit, faith-based hospital that relies on donations and volunteer surgeons to provide care to the underserved population of Kenya. The hospital could use your support no matter how big or small. Get more information here.
With countless needs and limited resources, there are many ways to contribute to the Kenya Initiative. Consider volunteering for the neurosurgery service at AIC Kijabe Hospital. Pediatric neurosurgeons and senior-level neurosurgery residents are invited to help provide clinical care and teaching. Second, consider offering financial support for Dan and Naomi as they complete their training in Cape Town. Lastly, there is an incredible need for medical equipment throughout the hospital. AIC Kijabe Hospital is a non-profit, faith-based hospital that relies on donations and volunteer surgeons to provide care to the underserved population of Kenya. The hospital could use your support no matter how big or small. Get more information here.
Visitors and contributors to the Kenya Initiative
|
Pediatric Neurosurgeons
Sandi Lam, Houston Nick Wetjen, Mayo Doug Cochrane, Vancouver Veetai Li, Buffalo John Collins, West Virginia Howard Silberstein, Rochester Cathy Mazzola, New Jersey Tom Steineke, New Jersey Jodi Smith, Indianapolis Bill Loudon, Orange County Patrick McDonald, Winnepeg Dan Couture, Wake Forest Nurses Kerri Kujak, Wisconsin Kristin Evans, Wisconsin Jenny Paul, Wisconsin Dianne Siebold, Indianapolis |
Pediatric Craniofacial Plastic Surgeons
Del Mount, University of Wisconsin Lisa David, Wake Forest Neurosurgery residents Lindsay Lipinsky, University of Buffalo Taylor Abel, University of Iowa Peter Bouz, Loma Linda Jennifer Strahl, University of Michigan Alireza Monsoui, Toronto Kimberly Foster, University of Pittsburgh Jonathan Forbes, Vanderbilt Luke Tomyz, Vanderbilt Rory Murphy, Washington University in St. Louis Wendell Lake, University of Wisconsin Brandon Rocque, University of Wisconsin Nunthasiri Wittayanakorn, Thailand Pediatric Neurosurgery Fellows Mark Van Poppel, Memphis Scott Wait, Memphis |



